
Protect Revenue. Reduce Risk.

Quickly analyze claims data to identify outlier billing patterns, revenue leakage, and coding habits that can trigger denials or audits
Find opportunities to improve documentation, accuracy and reimbursement
Specialty-Focused Accuracy
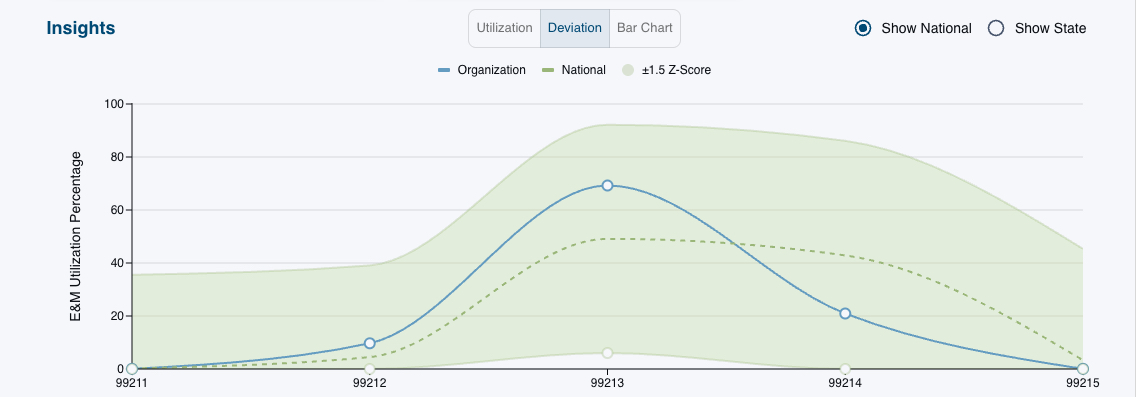
See how your providers compare to national specialty benchmarks and show you exactly where opportunities exist to improve documentation, accuracy, and reimbursement.
Spot Down-Coding Before It Hurts Revenue
Identify when payer behavior or coding patterns suggest downcoding or suppressed reimbursement, giving you the evidence you need to challenge decisions and protect revenue.
Backed by Compliance and Coding Experts
Specialty-focused insights that pinpoint the why behind performance trends, giving you clarity you can't get from generic analytics.
How SENTRY Works



Analytics
Audits
Education
Risk analytics are performed across all providers to identify outlier billing patterns and prioritize audit activity. These analytics ensure both existing and emerging risk is continuously monitored.
In the first quarter, one group of providers is audited based on this baseline risk profile. The following quarter, those providers receive targeted education while analytics are rerun, and a second group of providers (either the remaining providers or newly identified high-risk providers) are audited.

What SENTRY Really Means for Your Practice
Clarity and peace of mind.
Reduced audit risk
Revenue Recapture
From identifying downcoding and missed reimbursement
Fewer modifier-related denials
and cleaner claims
Clear priorities
for audits and education (no more guessing who to review)
Stronger compliance posture
with documented, ongoing oversight
